What is Humeral Interlocking Nail and Its Benefits?
The Humeral Interlocking Nail has become a crucial tool in orthopedic surgery. Dr. John Smith, a leader in orthopedic innovation, states, "This device transforms the way we treat humeral fractures." It’s designed to stabilize and promote healing effectively.
Patients recovering from humeral fractures often face lengthy rehabilitation. With the Humeral Interlocking Nail, surgery time reduces significantly. This nail offers better alignment and support during the recovery process.
However, challenges still exist. Some patients experience complications or delayed recovery. There are also concerns about the nail's material and the body’s response. Continuous research into improving its design is essential. As Dr. Smith emphasizes, "Innovation must never stop.
Definition and Overview of Humeral Interlocking Nail
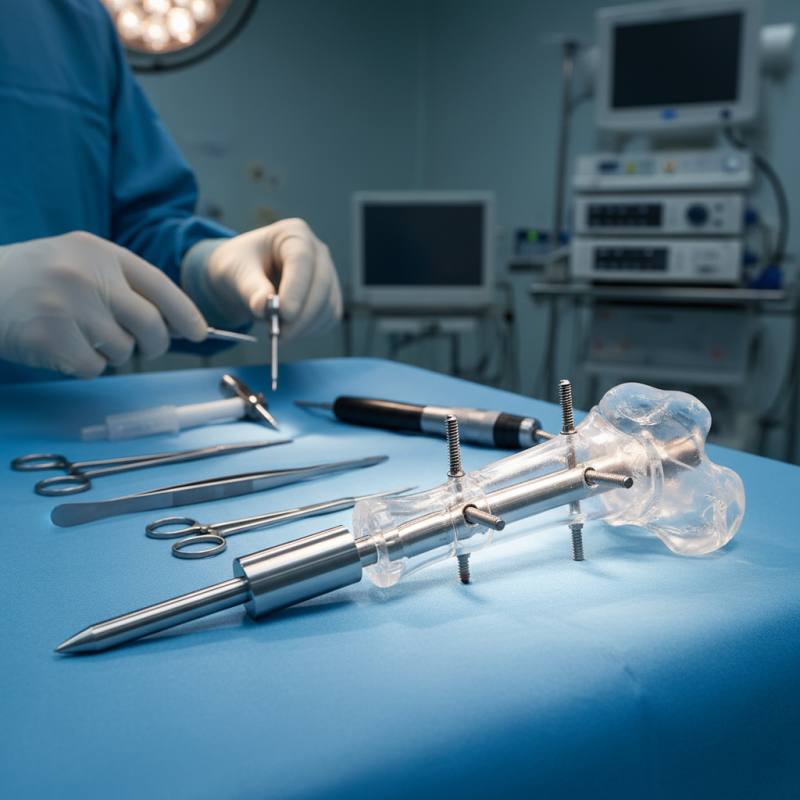
Humeral interlocking nails are specialized medical devices. They are designed for stabilizing fractured humerus bones. This technique is primarily used in orthopedic surgery. Surgeons insert these nails through the humerus, providing internal support. The interlocking feature secures the nail in place.
The benefits of using humeral interlocking nails are significant. They help reduce the risk of malunion or nonunion. Patients often experience quicker recovery times. These nails allow for early mobilization, promoting better outcomes. However, complications can arise, such as infection or improper alignment. Surgeons must carefully consider these risks.
In some cases, patients may feel discomfort after the procedure. Rehabilitation varies from person to person. Some may face challenges in regaining full range of motion. Understanding these aspects is crucial for both patients and healthcare providers. Each case presents unique challenges that need reflection and attention.
Indications for Humeral Interlocking Nail Usage
Humeral interlocking nails are increasingly used for treating humeral fractures. Their benefits are numerous, especially in complex cases. A recent study published in the Journal of Orthopedic Trauma indicates that these nails offer excellent fracture stability, leading to quicker patient recovery. The screws allow for immediate weight-bearing, a critical factor in rehabilitation.
Indications for using humeral interlocking nails include diaphyseal fractures and cases where traditional fixation fails. Additionally, they are ideal for patients with complex injury patterns. Research shows that this method reduces the risk of malunion and nonunion. However, not all cases are suited for this technique. Surgeons must carefully assess the fracture type and patient condition before choosing this approach.
The average healing time for patients using this method is approximately 12 weeks. Still, complications can arise, such as infection or hardware irritation. Monitoring for these issues is crucial for long-term success. While the humeral interlocking nail is effective, practitioners must remain vigilant and adaptable to each patient’s unique situation. Some patients may experience discomfort, emphasizing the importance of tailored post-operative care.
Surgical Procedure for Humeral Interlocking Nail Insertion
The surgical procedure for inserting a humeral interlocking nail involves several precise steps. The patient is positioned suitably to allow access to the humerus. An incision is made on the lateral side of the arm, exposing the bone. Clear visibility is crucial for successful placement.
Next, a guide wire is inserted into the humerus at the appropriate angle. This wire serves as a reference point for drilling. The surgeon carefully drills through the bone, ensuring stability. The interlocking nail is then placed over the guide wire. Screws are inserted to secure the nail, enhancing stability.
Despite its effectiveness, challenges may arise during the procedure. For instance, the risk of infection at the incision site remains. Aesthetic concerns may also surface; scars can form unexpectedly. Surgeons must remain vigilant, always ensuring the optimal alignment of the nail. Reflecting on these aspects can lead to better outcomes in future surgeries.
Benefits and Advantages of Humeral Interlocking Nail
Humeral interlocking nails are innovative tools used in orthopedic surgery. They offer significant benefits for patients with humeral shaft fractures. One major advantage is their ability to provide stable fixation. This stability promotes proper healing and diminishes the risk of malunion. Patients recover more effectively when their bones remain aligned.
Another benefit is the minimally invasive nature of the procedure. Surgeons insert the nails through small incisions. This approach reduces tissue damage and results in less pain post-surgery. Many patients appreciate a shorter recovery time and fewer complications. It’s essential to remember that not every case is ideal for this method. Some may have specific conditions that require alternative treatments.
There can be challenges with the technique as well. Proper alignment is crucial; bad positioning can lead to issues. Surgeons must have extensive training to navigate these risks. Despite these potential drawbacks, humeral interlocking nails remain a popular choice for treating complex fractures. The advantages often outweigh the risks when performed by skilled professionals.
Benefits of Humeral Interlocking Nail
Potential Complications and Considerations in Treatment
Humeral interlocking nails are increasingly used in orthopedic surgeries. They provide stabilization for complex humeral fractures. However, along with their benefits, there are potential complications that must be considered.
One significant concern is infection. Research indicates that the infection rate could be as high as 3-15% in surgical procedures involving intramedullary nails. Such complications can lead to prolonged recovery times and additional surgeries. Proper surgical techniques and sterile environments are crucial for minimizing this risk.
Another critical aspect is non-union or malunion of the fracture. Studies show that the rate of non-union can range from 5-10%. This may necessitate further interventions, which can increase healthcare costs. Patients need to be informed about the risks involved. Improved follow-up and patient compliance can help in reducing these complications.
